Retina
Diabetic Retinopathy
An ocular manifestation of diabetes, diabetic retinopathy is the result of weakening on the blood vessels within the lining of the inner eye called the retina and is the leading cause of blindness in American adults.
Vision symptoms are usually rare in the early stages of diabetic retinopathy, however, intermittent blur and seeing spots in the vision can be warning signs. Risk factors for diabetic retinopathy include, poorly controlled diabetes, hypertension, smoking, and being diabetic for ten years or more. Typically affecting patients who have had diabetes for ten years or more, the longer a person has diabetes, the higher his or her chances of developing diabetic retinopathy.
Annual eye exams are strongly recommended for all diabetic patients. At Cumberland Eye Care, our retina specialists use photography methods to detect retinal blood vessel problems and to monitor changes from exam to exam. There are multiple forms of diabetic retinopathy, and Dr. SMITH can determine your particular form. With one form, blood vessels may swell and leak fluid. In another, abnormal new blood vessels grow on the surface of the retina. Watch the video to learn more. If you have diabetes and are concerned about diabetic retinopathy, schedule an appointment with our doctors for a comprehensive eye exam and be sure to include it on your patient history form.
It is an ocular manifestation of diabetes, a systemic disease, which affects up to 80 percent of all patients who have had diabetes for 10 years or more. The longer a person has diabetes, the higher his or her chances of developing diabetic retinopathy.
Despite these intimidating statistics, research indicates that at least 90% of new cases could be reduced to diabetic retinopathy, which is damage to the retina caused by complications of diabetes and is the leading cause of blindness in American adults. y preventative monitoring during regular eye examinations and proper treatment.
There are multiple forms of diabetic retinopathy, and only your doctor can determine your particular form. With one form, blood vessels may swell and leak fluid. In another, abnormal new blood vessels grow on the surface of the retina.
In the early stages of diabetic retinopathy, many do not notice a change to their vision because there are little to no symptoms. If an eye doctor does not catch diabetic retinopathy early, one could sustain mild blurriness at near or in the distance, as well as floaters. In severe cases a sudden loss of vision may occur.
Unfortunately, Diabetic Retinopathy can result in permanent damage that cannot be reversed. However, if caught in time, prescribed treatments may slow development and prevent vision loss.
Concerned about the onset of diabetic retinopathy? Call and schedule a preventative eye examination today.
Retinal Tears and Detachments
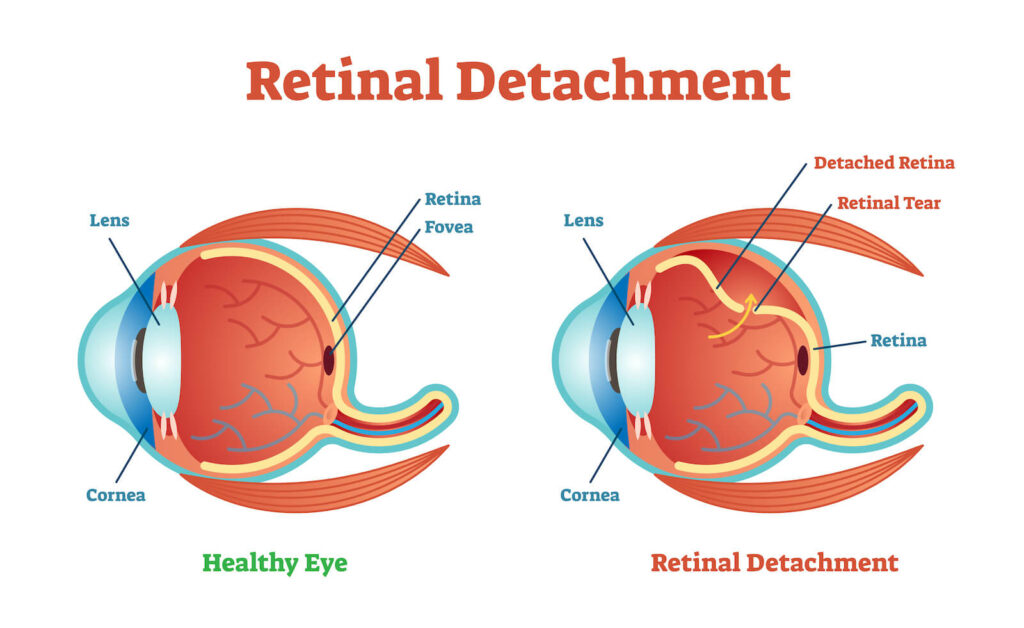
Retinal tears and detachments are conditions where the inner lining of the eye called the retina is damaged. The retina is a layer of tissue that’s light-sensitive and sends visual information through the optic nerve to the brain. If damaged, this layer of tissue can eventually detach from the inside of the eye, causing permanent vision loss.
A retinal tear describes a small break in this lining. Retinal tears can have many causes and can happen at any age. Retinal tears can be treated with laser surgery or an advanced “freezing” process. Both of these treatment options attempt to keep the retina in place and keep it from fully detaching.
Retinal detachment describes a much larger separation of the retina tissues and although it is not exclusive to older people, it’s more common in those over age 40. If detected with an eye exam early enough, retinal detachment can be treated with the procedures used for some tears, or with a more intricate surgery that uses gas to push the retina together with the wall of the eye to allow for reattachment.
Aging, eye trauma, eye surgery, or being drastically nearsighted may cause retinal tears or detachments. Symptoms of these retinal conditions may include seeing flashes or floaters, sudden blurry vision, and seeing an area of dark vision.
An eye exam is very important when these symptoms occur as permanent eyesight loss may occur if the retina problem is not treated in a timely manner.
Macular Degeneration
Age-related macular degeneration, often referred to as AMD, is a medical condition, which usually causes central vision loss in older adults. Macular degeneration can make it difficult or impossible to read or recognize faces, although enough peripheral vision remains to allow other activities of daily life.
AMD is not painful, which may allow it to go unnoticed for some time. Risk factors for macular degeneration may include smoking, obesity, Caucasian, female, and family history.
Having an annual eye exam is important for adults to allow our doctors to examine the macula and to measure vision. New research has shown that certain vitamins and proper sunglass protection for ultraviolet sunlight exposure may be helpful to lessen the risk of macular degeneration. Early diagnosis and continued observation by an eye doctor is crucial to protecting eyesight in macular degeneration patients.
Age-related macular degeneration, often referred to as AMD, is a medical condition which usually affects older adults. This vision-stealing disease is the result of degeneration to the macula and results in a loss of vision in the center of the visual field because of the damage to the retina. It occurs in dry and wet forms and is a major cause of blindness and visual impairments in adults over the age of fifty.
Macular degeneration can make it difficult or impossible to read or recognize faces, although enough peripheral vision remains to allow other activities of daily life. The dry form of advanced AMD results from atrophy of the retinal pigment epithelial layer below the retina, which causes vision loss due to the damage of photoreceptors also known as rods and cones in the central part of the eye.
The wet form of advanced AMD causes vision loss due to abnormal blood vessel growth ultimately leading to blood and protein leakage below the macula. Bleeding, leaking and scarring from these blood vessels eventually causes irreversible damage to the photoreceptors and rapid vision loss if left untreated. Fortunately, only about ten percent of patients suffering from macular degeneration have the “wet” type.
Macular degeneration is not painful which may allow it to go unnoticed for some time. For this reason, regular eye examinations are important. While approximately ten percent of patients age 66 to 74 will have findings of macular degeneration, the prevalence increases to thirty percent for patients age 75 to 85 years of age. Family history may also play a factor. The good news is that regular eye exams, early detection, and new treatment options enable doctors to maintain—and in some cases increase—visual acuity in patients.

